The #1 Heat Stress Prevention Wearable
SlateSafety’s armband measures critical safety data and alerts you in real-time
Trusted by Thousands of Workers at World-Class Organizations


Trusted by Thousands of Workers at World-Class Organizations
























Heat is the leading cause of death among all weather-related phenomena, and it is becoming more dangerous as 18 of the last 19 years were the hottest on record.
- Occupational Safety and Health Administration
The Problem
- Workers miss the warning signs of heat stress
- Supervisors are unsure who needs rest
- Organizations pay for costly injuries and have no actionable data
The Solution
- Workers manage their own work/rest cycles
- Supervisors can monitor and prevent overexertion
- Organizations keep their workforce safe and save money

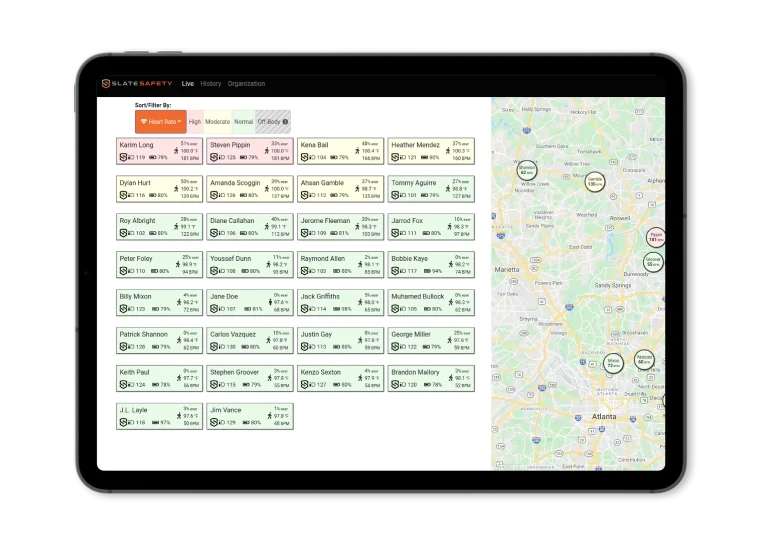
Personal Safety Monitoring
- Heat-illness prevention
- Real-time safety alerts
- Automated work/rest cycles
Lone Worker Support
- Emergency SOS alerts
- Fall and no-movement alerts
- Configurable behavior
Real-Time Location (RTLS) *
- Indoor worker location
- Outdoor worker location
- Incident localization
Environmental Monitoring *
- Ambient Temperature
- Relative Humidity
- Heat Index
How It Works
An intuitive, rugged and reliable system to prevent heat-illness in real-time

BAND V2 Wearable Solution
Each worker simply puts on our physiological monitoring device which assesses safety and sends real-time alerts.

Edge-based Cloud Architecture
In the cloud, data is securely processed and stored in compliance with SOC-2. Integrations are available via API.
Contact us for cloud alternatives.

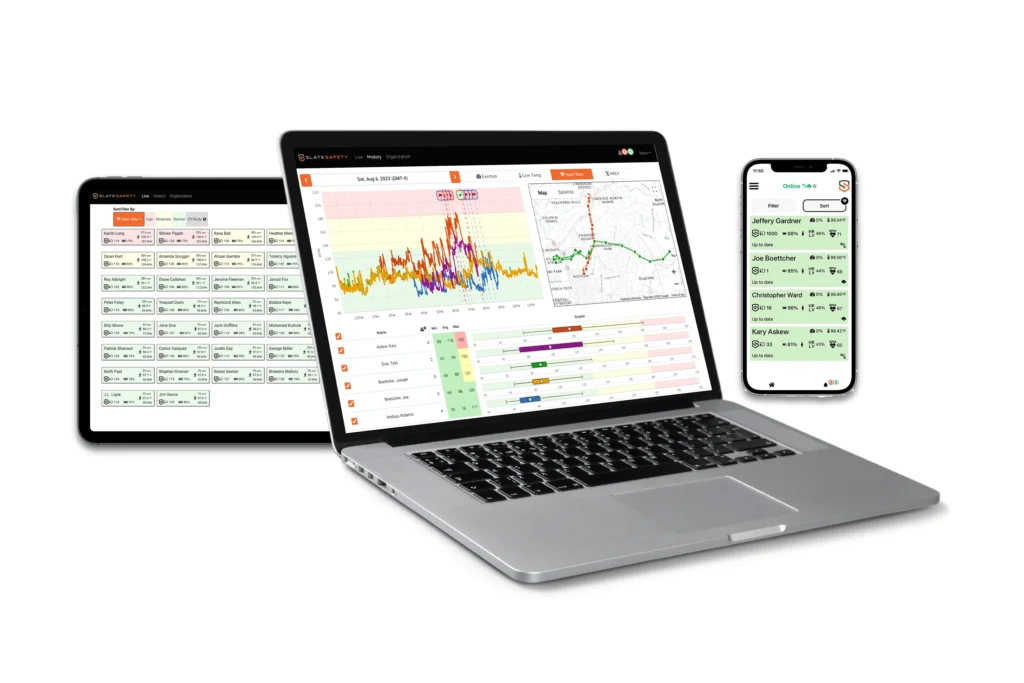
Web, iOS, and Android Application
Safety leaders can easily login to our web platform or mobile app to view real-time dashboards, configure alert thresholds and receive analytics.

Each worker simply puts on our physiological monitoring device which assesses safety and sends real-time alerts.
In the cloud, data is securely processed and stored in compliance with SOC-2. Integrations are available via API.
Contact us for cloud alternatives.
Safety leaders can easily login to our web platform or mobile app to view real-time dashboards, configure alert thresholds and receive analytics.
Introducing: The BEACON V2
Environmental monitoring for heat stress integrated seamlessly with the SlateSafety system.
The BEACON V2 focuses on ambient temperature monitoring to enhance heat safety programs.
It measures real-time temperature, relative humidity, and heat index it maintains SlateSafety requirements for reliability and durability.
Introducing: The BEACON V2
Environmental monitoring for heat stress integrated seamlessly with the SlateSafety system.
The BEACON V2 focuses on ambient temperature monitoring to enhance heat safety programs.
It measures real-time temperature, relative humidity, and heat index it maintains SlateSafety requirements for reliability and durability.

Enterprise-Grade Security and Privacy
We are committed to protecting the security and privacy for our customers. That is why we exceed industry standards and why the SlateSafety platform is penetration tested regularly.
We work directly with IT teams to accelerate system integration. Our customers also receive access to enterprise necessities such as IP whitelisting, multi-factor authentication, single sign-on, and more to fit their security needs.
An ACGIH® Partner
SlateSafety is a proud partner of the American Conference of Governmental Industrial Hygienists.
In fact, ACGIH’s recommended safety thresholds for preventing heat illness are built in to SlateSafety’s platform. It has never been easier to avoid heat injuries in compliance with ACGIH® TLVs and BEIs.
Smart PPE
SlateSafety’s wearable armband provides alerts for heat stress and overexertion so you can stop guessing how your team is doing and focus on the task at hand. Sensors measure data including heart rate, core body temperature, exertion and more using real-time and easy-to-use wearable technology.









